If your child is active and coming home with knee pain after sport, it’s worrying, but it’s also extremely common. In most cases there’s a clear, treatable explanation. Here’s what you need to know.

The Most Common Cause: Osgood Schlatter Condition
The most common cause of knee pain in active children, especially between the ages of 9 and 15, is Osgood Schlatter condition. (It’s sometimes referred to as “Osgood Schlatter disease,” although that term is misleading because it is not actually a disease.)
Osgood Schlatter is a growth related overuse condition that affects the front of the knee, just below the kneecap. The bony bump in this area is called the tibial tubercle, where the patellar tendon attaches to the shin bone.
During growth spurts, bones often lengthen faster than muscles and tendons can adapt. This creates repeated pulling forces at the point where the patellar tendon inserts into the tibial tubercle. In growing children, this attachment site is still developing and consists of a softer area of cartilage known as an apophysis, a type of growth plate, making it more vulnerable to stress than mature bone.
Repeated strain on this growth plate leads to irritation and inflammation, a process known as apophysitis, which is the underlying cause of Osgood Schlatter condition.
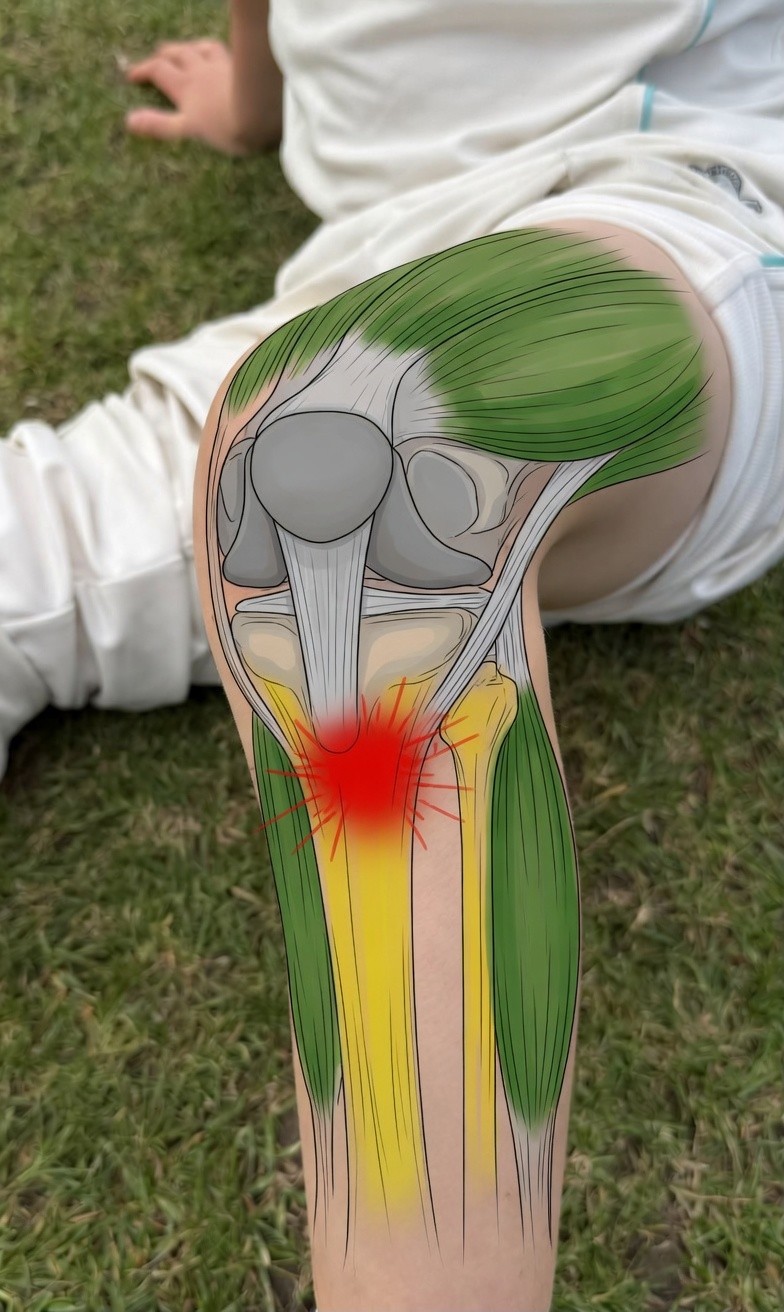
Colour key:
Green = quadriceps muscle
Yellow = tibia
Grey = knee cap (patellar tendon)
Red = site of pain at the tibial tubercle apophysis
The quadriceps muscle (green) contracts powerfully with every jump, sprint, and kick, pulling through the patellar tendon (grey) and via the kneecap (grey). In a growing child, the tendon inserts not into hard bone but into the tibial tubercle apophysis, a cartilaginous growth plate. Repeated traction on this soft growth plate causes inflammation and pain at the point marked in red. This process is called apophysitis, and it is the underlying mechanism of Osgood-Schlatters.
Classic Signs of Osgood-Schlatters
• Pain and tenderness just below the kneecap, not in the joint itself
• A visible or palpable bony lump below the knee that is sore to touch
• Pain that worsens during or after activity, especially running, jumping, kneeling, and stair-climbing
• Pain that eases with rest
• More common in boys aged 10 to 15, but increasingly seen in girls as sport participation has risen
• Can affect both knees, though one is typically worse than the other
The reassuring news: Osgood-Schlatter readily resolves completely once your child has finished growing. It’s a condition of growth, and growth, by definition, ends.
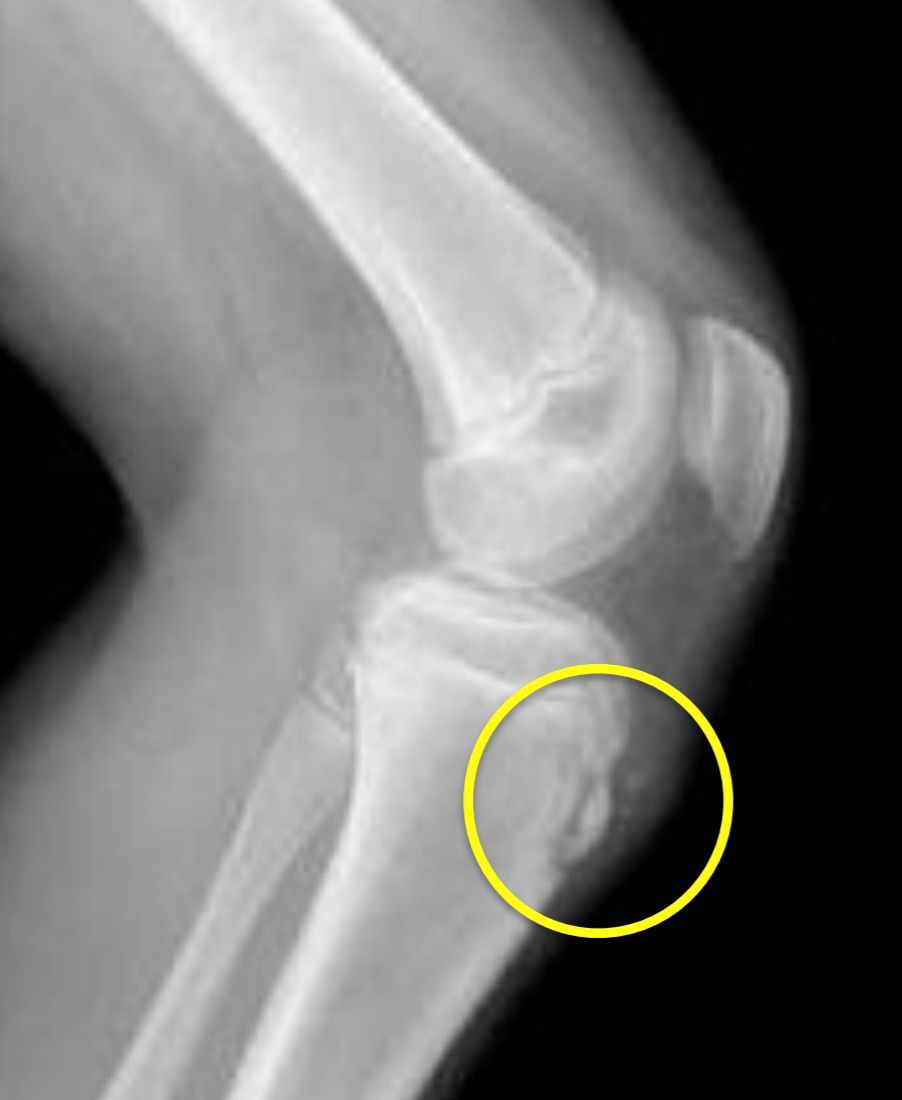
Lateral X-ray of a child’s knee showing fragmentation of the tibial tubercle apophysis highlighted with a yellow circle.
Other Causes of Knee Pain After Sport in Children
While Osgood-Schlatter is the most common culprit, there are several other conditions worth knowing about, and some are important not to miss.
Pain Syndrome, Runner’s Knee Pain - Around or behind the kneecap, caused by the kneecap not tracking smoothly in its groove during movement. Typically worse going downstairs, squatting, or sitting for prolonged periods with knees bent. Particularly common in teenage girls and in children who have recently increased their training load.
Sinding - Larsen-Johansson Syndrome - Similar to Osgood-Schlatter but affecting the lower pole of the kneecap rather than the tibial tubercle below it. Also growth-related, also self-limiting, and managed in much the same way.
Hypermobility Children - with naturally loose joints place extra demand on surrounding muscles during sport. This can cause aching, fatigue, and knee pain, often worse during activity and the day after, due to the additional muscular work required to stabilise the joint.
Pain Referred From the Hip : Do Not Miss This - This is one of the most important points I make in clinic: knee pain in a child is not always coming from the knee. Conditions such as Perthes disease typically in 5 - 10 yr olds or a slipped upper femoral epiphysis (SUFE) typically in 10-15 yr olds can present primarily as thigh or knee pain. This is why a thorough assessment that examines the hip as well as the knee is essential and should never be skipped.
Red Flags
Seek Assessment if your child has any of these:
• Pain that is severe or rapidly worsening despite rest
• Swelling, warmth, or redness around the knee joint
• Your child is limping or reluctant to put weight through the leg
• The knee locks, catches, or gives way
• Pain began after a specific injury or fall
• Pain has not improved after 4 to 6 weeks of modified activity
• Your child has stopped enjoying sport they previously loved
• Pain that is worse in the morning or present at rest
How Is Knee Pain After Sport in Children Managed?
For most growth-related causes, the initial focus is on sensible load management, which does not mean stopping sport entirely. Finding the right balance between activity and recovery is key, and I always work with families to keep children as active as possible while the condition settles. A structured physiotherapy programme targeting quad and hamstring flexibility, hip strength, and lower limb biomechanics makes a significant difference in the majority of cases. Ice after activity, appropriate footwear, and short-term pain relief where needed complete the conservative approach.
My assessment always begins with a thorough history and a clinical examination, looking not just at the knee but at the whole lower limb, including the hip. From there, I can organise any imaging that is necessary to finally give you a clear diagnosis, a realistic prognosis, and a tailored plan to get your child back to doing what they love.
Nev is one of the only surgeons in the UK with expertise in knee problems across all ages, from newborns to the elderly. He has been a Consultant at the Royal Berkshire Hospital since 2010 and completed a specialist children’s orthopaedic fellowship at Westmead Kids Hospital, Sydney. He consults privately at Spire Dunedin Hospital and Circle Hospital in Reading, The Princess Margaret Hospital In Windsor and at the world famous Fortius Clinic in London.

