Information for Families – Overriding 5th toe
Nev Davies
Reading Children’s Orthopaedic Unit
What is an overriding 5th Toe?
This uncommon condition is usually present at birth but can become more noticeable in the first few years. The 5th little toe sits on top of the 4th toe, curling inwards. Sometimes it occurs just in one foot, sometimes in both.
What are the symptoms of an overriding 5th Toe?
The main concern is the look of the toe, but in many people these toes don’t cause too many problems. Sometimes, symptoms such as rubbing, hard skin, blistering or pain can occur, as well as difficulties getting shoes to fit.
What causes this?
We do not know exactly what causes the toe to sit like this. Although it has been noted that the condition can affect several generations, which implies that it is sometimes passed on from parent to child (inherited).
What is the natural history of this condition?
If the foot remains asymptomatic (no symptoms) and pain free we tend to observe and leave well alone. We would encourage moisturisation after baths and wide fitting shoes for comfort.
How can it be treated?
Treatment options are quite binary.
Option A. Leave alone and observe. We tend to do this in asymptomatic or patients who present noticeably young (under the age of 4).
Option B. Surgery to straighten the toe. If the toe does become symptomatic, surgery is usually advised before school age. The operation is done under a general anaesthetic as a day case procedure. At the time of consent, we would discuss the procedure in detail with you, including the benefits and the risks of the surgery, as well as the post-operative care. Please see the separate information leaflet regarding surgery.
Surgical Reconstruction
What does the operation involve?
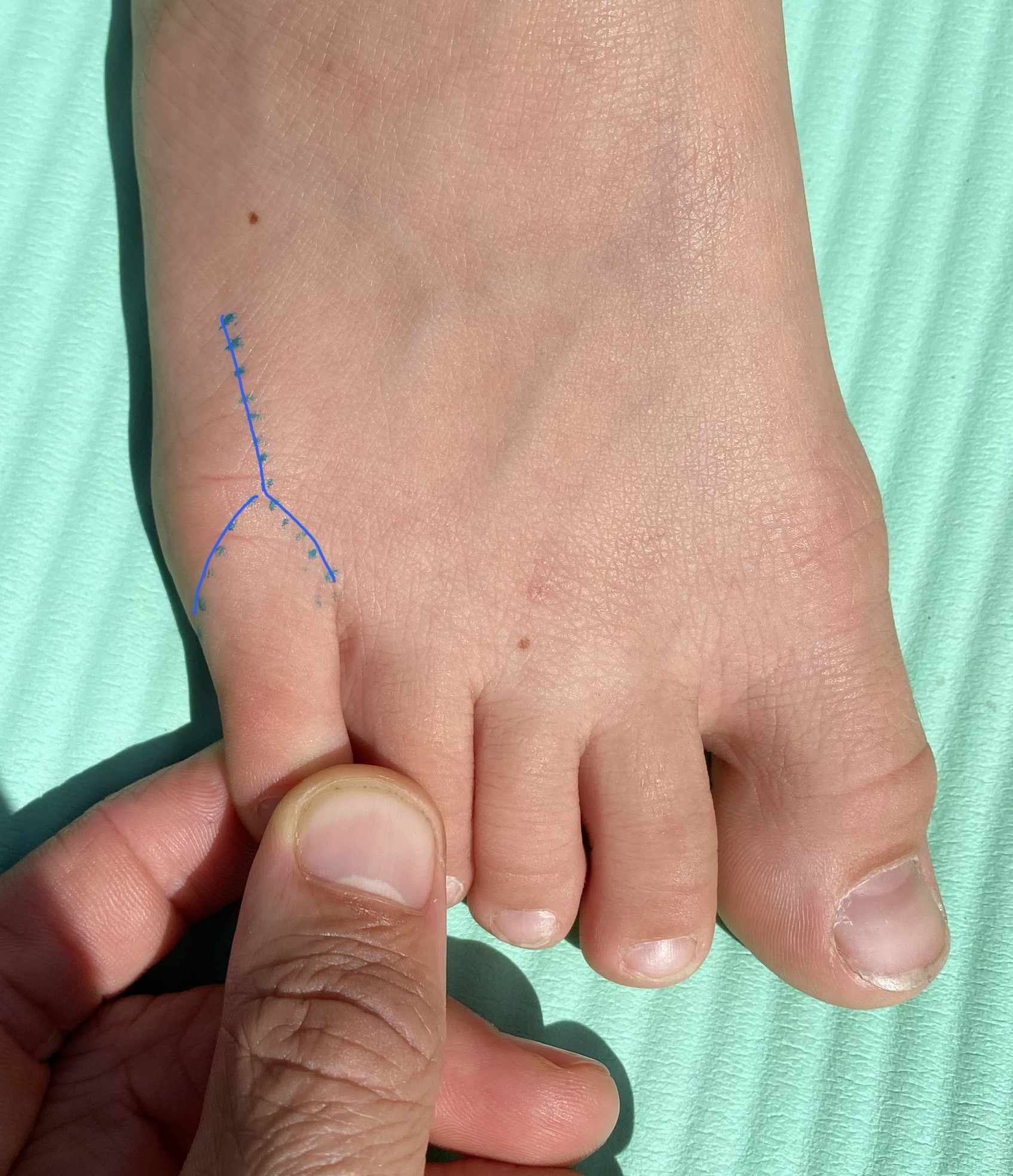
The operation is done under a general anaesthetic as a day case procedure. We also numb the toe with local anaesthetic. It is quite a big operation through a large scar (see blue line on photo.) It requires a large soft tissue release of all the tight structures to get the toe straight. Dissolvable stitches are used as well as paper stitches and a big wool and crepe dressing is applied.
What is the aftercare?
It is extremely important to elevate the foot for 72 hours after the operation. This helps the swelling settle and to aid healing. A temporary splint (half plaster) with a heel-walking shoe is used. Crutches are useful to get around, but not essential, particularly at school. Patients are seen in clinic around 2 weeks after the operation to check the scar is healing and to redress the wound. Most patients would slowly wean into a shoe with a nice wide toe box at this stage. Return to sports and activities is at around 4-6 weeks.
What are the success rates?
Most families are very happy with the result. There is always a small chance of recurrent tightness, usually due scar tissue build up and the toe reverts to its overriding position. In these cases, I would refer to a plastic surgeon for an additional opinion.
What are the risks of surgery?
The risks of surgery are small and include the general surgical risks of any surgery. These include infection, ugly scar and skin numbness. The more specific risks of this operation include recurrent deformity, tendon damage and loss of blood supply to the toe. I will discuss all this in detail with you before we proceed.








