Accessory Navicular Bone – Information for Families
Parent Information Series – Nev Davies
Reading Children’s Orthopeadic Unit
Information for Families – Accessory Navicular Bone
What is an accessory navicular?
An accessory navicular is an extra bone (ossicle) which is found next to the navicular bone (one of the bones on the inside of the foot). It is the most common extra bone in the foot occurring in between 4-14% of the population.
What is the cause?
This condition tends to run in families so may have a genetic basis.
What are the symptoms?
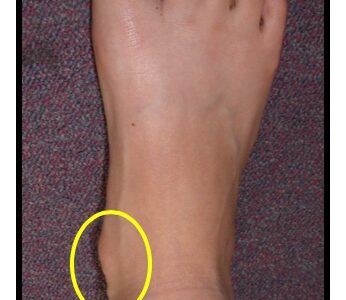
It can cause problems in young patients and is often related to having flat feet. The bump can become red and sore as it causes rubbing on the inside of shoes.
How is it diagnosed?
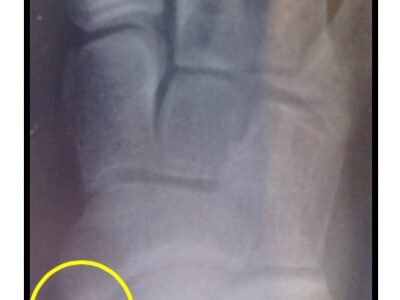
It is typically easy to feel the bump, but the diagnosis is confirmed with an X ray – see yellow circle shown.
What is the natural history?
In most cases, people who have these extra bones do not have any symptoms like rubbing. In those patients who do have symptoms, they seem to come and go as they tend to be activity related.
What are the treatments?
Non operative treatment – These are always tried first and often relieve symptoms:
- Restricting those particular activities (i.e. certain sports) that aggravate symptoms
- Custom made insoles (orthotics) to fit inside shoes. The purpose of these is to take pressure off that area
- Physiotherapy to strengthen the muscles across the foot (tibialis posterior muscle)
- A below knee walker boot or plaster cast is sometimes used for 2 weeks to rest the foot and let any associated inflammation settle right down
Interventional Treatment – If patients’ symptoms persist after a good time period of the above options, then often an MRI scan will be organised to confirm that the extra bone (assessor navicular) is inflamed. If the MRI confirms this, there is an option to try an ultrasound guided injection of steroid into that area. This is performed by the consultant radiologist.
Operative Treatment – If after a period of several months, non-operative treatments have not helped, then surgery is considered. Please see the separate patient information leaflet on surgery.
Operation for Accessory Navicular Bone
What is involved with the operation?
The operation is straightforward and is done as a day case, under a general anaesthetic. (Please also watch this YouTube video to help you prepare). It involves removing the additional bone through a small scar over the bump, on the inside of the foot.
What is the aftercare?
It is really important to elevate the foot for 72 hours after the operation to help the swelling settle and to aid healing. I use a temporary splint (half plaster) with a heel-walking shoe. Crutches are useful but not essential to get around, particularly at school. I see patients at 2 weeks after the operation in clinic to check the scar is healing, to organise some new insoles and start physiotherapy. Physiotherapy should continue for several weeks to strengthen the foot, ankle and calf. I would anticipate a return to running at 4-6 weeks and contact sports at 8-12 weeks.
What are the success rates and risks?
The surgery has a success rate of about 90% in taking the symptoms away completely. The risks of surgery are small and include the general surgical risks of infection, ugly scar, numbness in addition to specific risks of this operation including ongoing pain, and tendon damage. I will discuss this in detail with you. The vast majority of patients do well and return to pain free activities after 3-4 months.
If you have any questions, please don’t hesitate to contact us!