Exostosis (Osteochondroma) – Information for Families
Nev Davies
Children’s Orthopaedic Consultant
Reading Children’s Orthopeadic Unit
Information for Families – Osteochondroma (exostosis)
What is an Osteochondroma ?
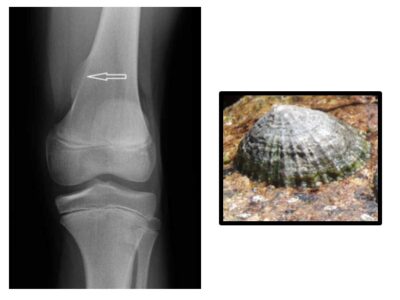
An osteochondroma or exostosis is a benign bony lump with a cartilage cap that arises usually at the end of the long bones. They come in various shapes and sizes and are usually found next to the growth plates of the distal femur (end of the thigh bone) or proximal tibia (top of the shin bone) (see picture 1) around the knee. They are the commonest bony lump and occur in approximately 1 in 50,000 people, although this is probably an underestimated figure as many may go unnoticed.
What is the cause?
These lumps (if you have lots of them) can run in families with a condition known as Multiple Hereditary Exostoses or diaphyseal aclasis, which has a genetic basis, but the vast majority of solitary (single) lumps are sporadic (occur at random).
What are the symptoms?
Sometimes they do not cause any symptoms at all, but they can be painful particularly if knocked or banged playing sports. Occasionally they can cause inflammation of the tendons running close by.
How are they diagnosed?
It is typically easy to feel the lump which is hard and feels like bone. The diagnosis is confirmed with an X-ray. Occasionally an ultrasound scan, a CT scan (3D X-ray) or an MRI scan is used to look at the lump in more detail. The lumps can be sessile (like a limpet on a rock (see picture 2 plain X-ray)) or pedunculated like a floret of broccoli. (See picture 3 (CT 3d Reconstruction))
What is the natural history?
A lot of people who have these lumps are asymptomatic. This means they have no symptoms. In those unlucky patients who do have symptoms, they tend to continue, unless the lump is removed. The lumps grow as the patient grows. When the skeleton stops growing, usually age 13 in girls or age 15 in boys, the lump also stops growin
What are the treatments?
Non-operative treatment is always tried first and includes confirming the diagnosis with imaging and then an explanation about the natural history of the lumps, usually followed by a period of observation.
If after a period of several months symptoms worsen, then an operation to remove the lump (surgical excision) is considered.
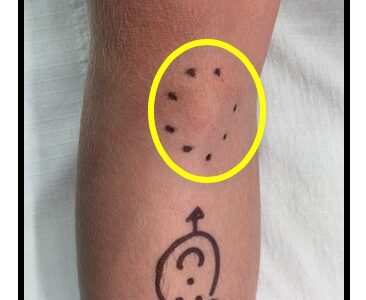
What is involved with the operation?
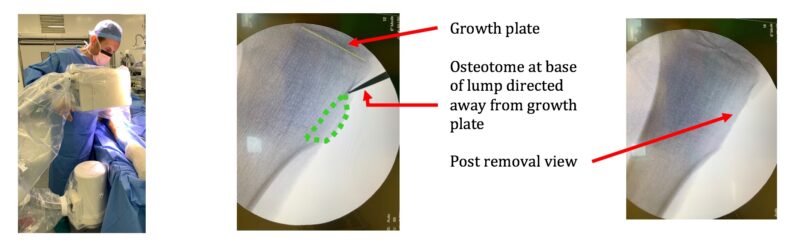
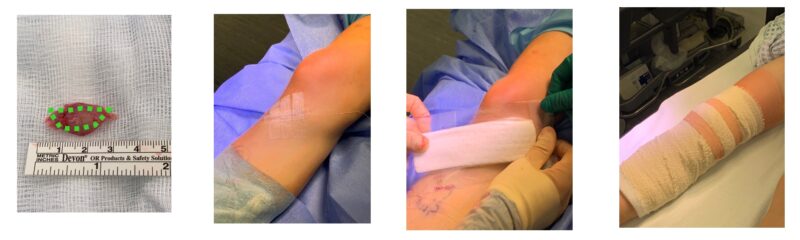
The operation is usually straightforward and involves removing the lump level to the bone. It involves a general anaesthetic (you are fully asleep) and usually done as a day case. Through an incision over the lump, it is then removed level to the bone. The lump is sent off to the laboratory to be analysed under the microscope to check it is an Osteochondroma and not anything else.
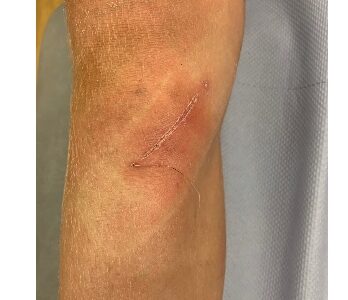
The surgery has a high success rate in removing the symptoms, with very little risk involve. Dissolvable stitches are used under the skin and paper stitches over the top. A special waterproof dressing is applied, and a wool and crepe bandage is used to help reduce swelling.


What are the risks of the operation?
The risks of the operation are few but can be divided into general risks of any surgery and more specific risks to this particular procedure. The operation is straight forward taking between 30 minutes to an hour to do.
General risks include:
- infection
- wound splitting and a widened scar
- numbness
- bleeding and bruising
- swelling and stiffness
- fracture
Specific risks include:
- incomplete removal
- recurrence
- growth plate damage (if near the growth plate)
What happens after the operation?
It is important to rest up for a few days and keep the leg elevated on pillows to maximise healing in the first week. This encourages the soft tissues to settle and prevents ongoing bleeding and bruising. Using ice packs and doing gentle knee exercises can also aid recovery.
Further Follow Up
It will be arranged for you to be seen at about 2 weeks after the operation to check that the scar is healing well, and everything is slowly improving. It is normal for there to be some residual swelling and bruising at this time and it may take a few weeks more before returning to normal sports and activities. Sometimes some physio is needed to help get the joint moving and the muscles to recover, but it would usually take about 6 weeks in total to return to normal.
We arrange a final check and an x-ray of the area at about 6 months after the operation to check the growth plate is growing well.